Detecting Drug-Induced Hyperpigmentation: A Clinical Guide
Overview
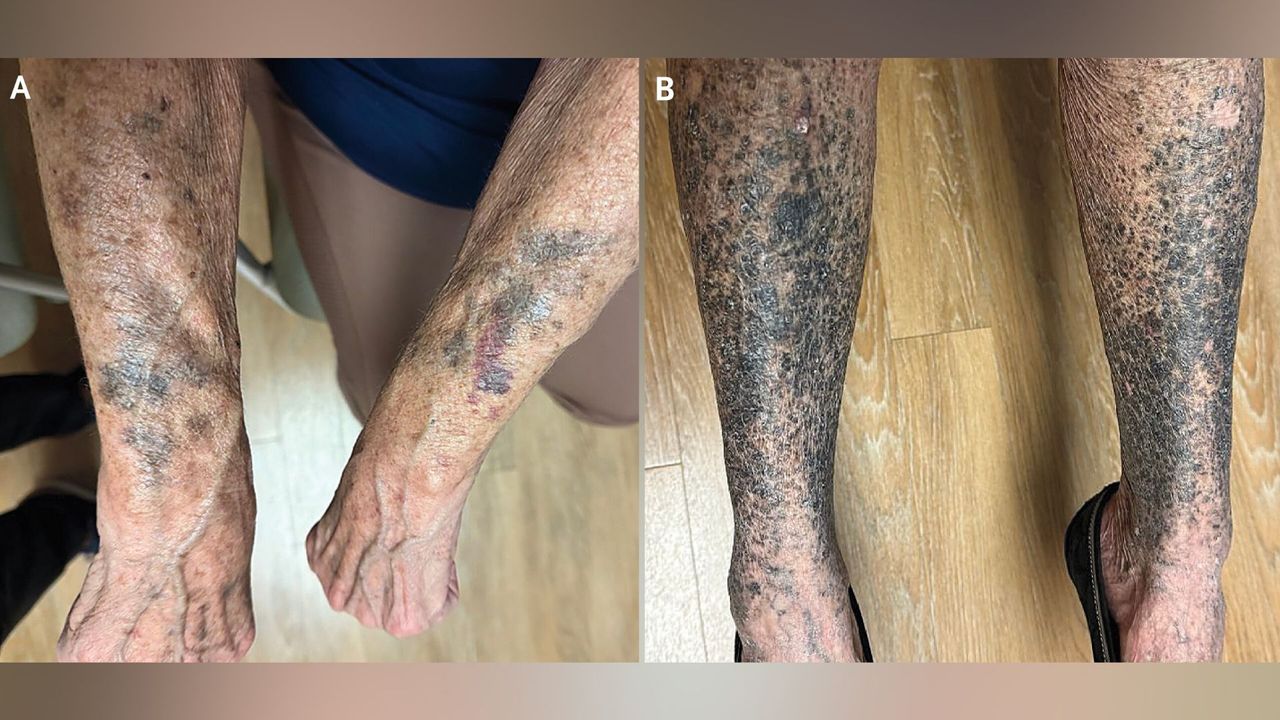
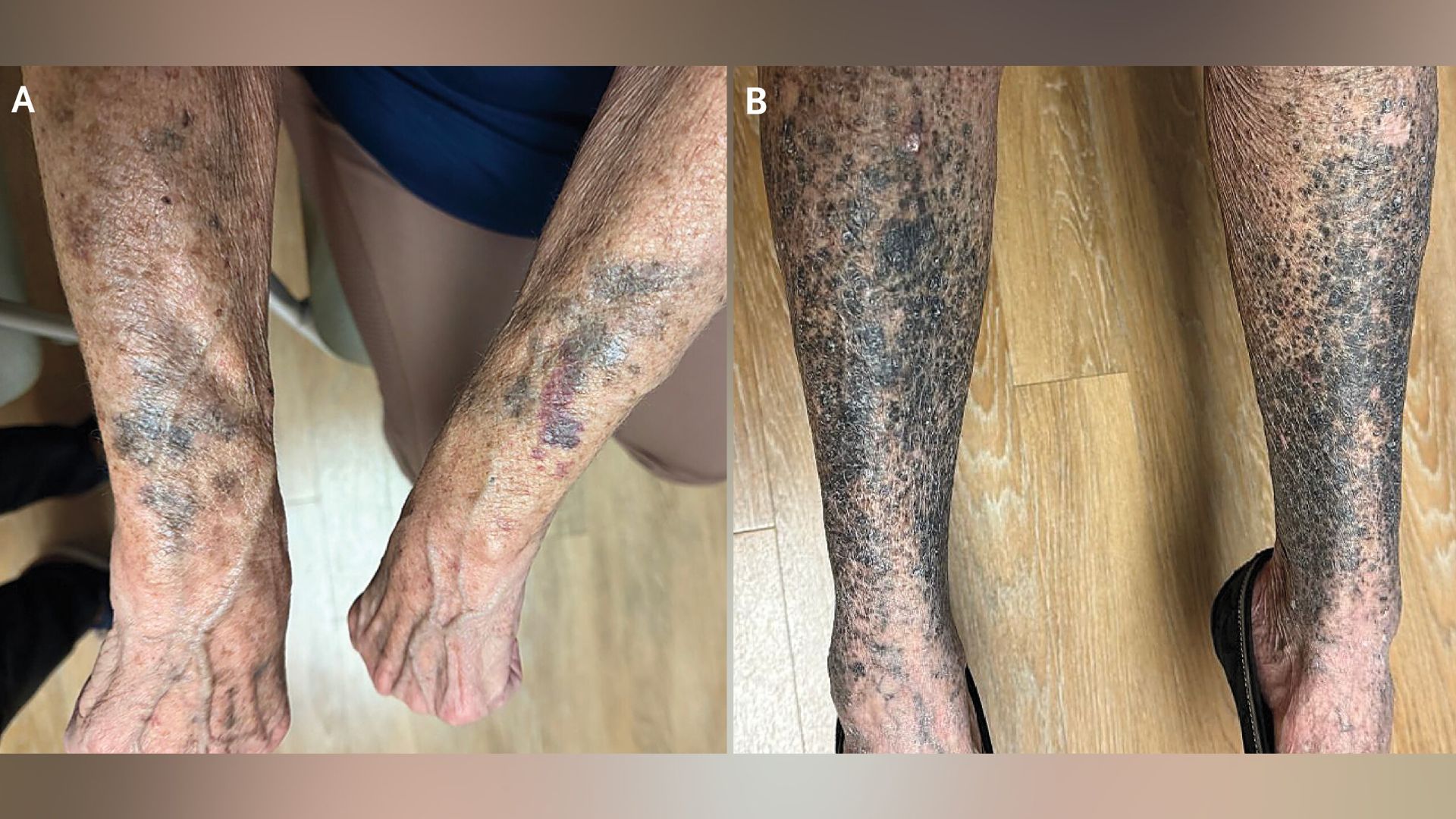
Hyperpigmentation—where patches of skin become darker than the surrounding area—can arise from many causes, including sun exposure, hormonal changes, or skin injuries. One often overlooked trigger is medications. The case of a woman who developed striking black-and-blue discoloration weeks after starting a new drug highlights a classic diagnostic dilemma: distinguishing drug-induced hyperpigmentation from other pigmentation disorders. This guide provides a structured approach to recognizing, diagnosing, and managing medication-related skin darkening, focusing on the clinical clues that set it apart from conditions like melasma, post-inflammatory hyperpigmentation, or systemic diseases.
Prerequisites
Required Knowledge
- Basic understanding of skin anatomy and pigmentation (melanocytes, melanin)
- Familiarity with common hyperpigmentation disorders (e.g., melasma, lentigines, acanthosis nigricans)
- General knowledge of pharmacotherapy and adverse drug reactions
Tools & Resources
- Patient medication list (including OTC drugs, supplements, and topical agents)
- Wood lamp (Wood’s light) for examining pigment depth
- Dermatoscope (optional, for detailed evaluation)
- Biopsy kit and pathology lab access (if needed)
- Drug reaction databases (e.g., PubMed, Micromedex)
Step-by-Step Diagnostic Approach
1. Identify the Pattern and Onset of Hyperpigmentation
Drug-induced hyperpigmentation often follows a specific timeline and distribution. Ask the patient:
- When did the discoloration begin? Typically weeks to months after starting the offending drug.
- Where is it located? Many medications cause photodistribution (sun-exposed areas like face, neck, arms). Others produce fixed patterns (e.g., amiodarone gives slate-gray on face, antimalarials cause blue-black on shins).
- Color and morphology: Is it brown, blue-black, gray, or purplish? The hue can hint at the drug class. For instance, minocycline often leaves blue-black macules on legs or in scars; NSAIDs may cause photosensitive hyperpigmentation with preceding inflammation.
2. Review the Medication History Thoroughly
Create a comprehensive timeline of all drugs, including start and stop dates. Common culprits include:
- Antimalarials (chloroquine, hydroxychloroquine)
- Amiodarone
- Tetracyclines (especially minocycline, doxycycline)
- NSAIDs (e.g., indomethacin, piroxicam)
- Antipsychotics (phenothiazines like chlorpromazine)
- Chemotherapeutic agents (bleomycin, cyclophosphamide)
- Hormonal therapies (oral contraceptives, hormone replacement therapy)
- Heavy metals (silver, gold, bismuth—though less common today)
Cross-reference the onset with any drug initiation or dose change. If multiple drugs are involved, consider synergism (e.g., tetracyclines plus antimalarials increase risk).
3. Perform a Targeted Physical Exam
- Wood lamp examination: Drug-induced pigmentation often shows accentuation under Wood’s light if melanin is in the epidermis (brown-black). Dermal pigmentation (due to drug-metal complexes or deeper deposition) may not fluoresce.
- Check mucous membranes: Some drugs (e.g., antimalarials, minocycline) can affect oral mucosa, gums, or conjunctiva.
- Note associated signs: Look for preceding erythema, blistering, or pruritus that might suggest a photosensitivity reaction.
4. Consider Differential Diagnoses
Rule out other causes of sudden hyperpigmentation using a systematic approach:
- Post-inflammatory hyperpigmentation (PIH): History of preceding rash, trauma, or inflammation in the same area.
- Melasma: Symmetrical, usually on face; associated with pregnancy, oral contraceptives, or sun exposure.
- Addison’s disease: Generalized hyperpigmentation plus fatigue, hypotension, and electrolyte abnormalities.
- Hemochromatosis: Bronze discoloration with diabetes, liver disease, and elevated ferritin.
- Nail or scleral pigmentation: May indicate heavy metal deposition or systemic drugs like doxycycline.
5. Perform Diagnostic Tests (If Indicated)
When history and exam are not conclusive:
- Skin biopsy: Send for routine histology (H&E) and possibly special stains (e.g., Perl’s for iron, Fontana-Masson for melanin). Drug deposits (e.g., amiodarone lipofuscin, minocycline iron complexes) may be visible as yellow-brown granules in macrophages or dermis.
- Blood tests: Check complete blood count, iron studies, cortisol, ACTH, and metabolic panel if Addison’s or hemochromatosis is suspected.
- Photo-testing: If photosensitivity is suspected, minimal erythema dose (MED) testing can confirm.
6. Establish Causality and Withdraw the Suspected Drug
Use the Naranjo adverse drug reaction probability scale or the WHO-UMC causality assessment. Definite proof often requires re-challenge, but in practice, stopping the drug is the main step.
- For immediate benefit: Advise sun protection (broad-spectrum SPF 30+, protective clothing).
- Treat residual pigmentation: Topical agents (hydroquinone, tretinoin, vitamin C), chemical peels, or laser therapy (Q-switched laser for dermal pigmentation).
- Monitor resolution: Pigmentation may fade over months to years; some drugs (e.g., minocycline, amiodarone) cause permanent changes.
Common Mistakes
Mistake #1: Blaming the Wrong Drug
Patients often take multiple medications. Do not assume the most recently started drug is the culprit. Some drugs (e.g., amiodarone) cause delayed pigmentation up to a year after initiation. Always create a timeline and consider cumulative effects.
Mistake #2: Overlooking Over-the-Counter and Topical Agents
Many people do not list supplements, herbal products, or topical steroids. Ask specifically about these. For example, hydroquinone creams can cause exogenous ochronosis (blue-black pigmentation).
Mistake #3: Forgoing a Biopsy When Needed
If the pigmentation is atypical or not resolving, a biopsy can differentiate drug-induced pigmentation from melanoma or atypical nevi. Delaying this can lead to misdiagnosis.
Mistake #4: Failing to Document Photosensitization
Many drug-induced hyperpigmentations are phototoxic in nature. Advise strict sun avoidance from the start. If the patient is already pigmented, continued sun exposure can worsen the condition.
Mistake #5: Not Re-evaluating After Drug Withdrawal
Some clinicians assume pigmentation will disappear quickly. In reality, it may persist for months or permanently. Re-evaluate after 3–6 months and consider referral to dermatology if no improvement.
Summary
Drug-induced hyperpigmentation is a reversible but often underdiagnosed adverse event. A careful history of medication timing, physical exam with Wood lamp, and targeted tests can identify the cause. The mainstay of management is discontinuation of the offending drug, followed by sun protection and adjunctive therapies. With a systematic approach, clinicians can avoid diagnostic errors and improve patient outcomes.